Scientists in Australia developed a groundbreaking biological strategy to fight Dengue fever — a mosquito-borne viral illness that strikes over 50 million people each year, causing severe fevers, debilitating joint pain, and in some cases death. Despite killing far more people globally than influenza, Dengue rarely receives proportionate attention in Western media coverage.
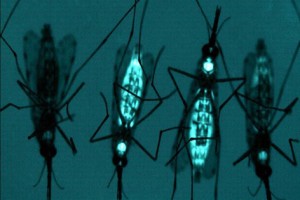
Their approach centers on a naturally occurring bacterium called Wolbachia pipientis, which infects many insect species and has a remarkable ability to alter its host’s reproductive biology. When introduced into mosquitoes, Wolbachia nearly eliminates their capacity to transmit the Dengue virus to humans. The infected mosquitoes spread the bacterium through natural reproduction, eventually replacing wild disease-carrying populations without any ongoing human intervention.
Field trials in two towns in northern Australia demonstrated dramatic results. Researchers released between 10,000 and 20,000 Wolbachia-carrying mosquitoes, and infection rates among the wild population approached 100 percent — effectively replacing nearly all disease-transmitting mosquitoes with harmless ones.
This biological approach stands in stark contrast to the genetically engineered mosquitoes being produced by Oxitec, a UK-based biotechnology firm that had already released millions of laboratory-modified insects into multiple countries, often without adequate public awareness or consent.
Why Dengue Fever Deserves More Attention Than Influenza
Dengue has been spreading faster than any other insect-borne viral disease worldwide, threatening populations in more than 100 countries and putting an estimated 2.5 billion people at potential risk. The infection produces intense fever, crushing headaches, severe eye pain, skin rashes, and agonizing skeletal pain so extreme that it earned the nickname “breakbone fever.” The more severe variant, Dengue hemorrhagic fever, can be fatal.
Once confined to tropical regions, Dengue has expanded its geographic range considerably. Cases have been documented in Texas, Florida, and other southern US states, and the disease has reached endemic status in 125 countries. Central America has experienced full-scale epidemics.
The primary mosquito vectors are Aedes aegypti and, to a lesser extent, Aedes albopictus, both of which thrive in tropical and subtropical climates — the same regions where malaria is prevalent. International travelers who visit affected areas can also carry the virus back to their home countries.
The numbers tell a striking story: while influenza produces roughly three to five million cases annually worldwide, Dengue generates approximately 100 million — a ratio of roughly 20 to 1. All four known Dengue virus serotypes are now circulating in the Americas.
Traditional prevention efforts focused on community-based mosquito control programs with minimal chemical pesticide use. However, the emergence of high-tech biological and genetic strategies has fundamentally changed the landscape of Dengue prevention — though not all of these new approaches carry the same risk profile.
Safety Questions Surrounding Wolbachia-Based Mosquito Modification
Some scientists initially raised concerns about introducing bacterially infected mosquitoes that interact with human blood. Researchers involved in the Wolbachia program have maintained that the bacterium poses zero risk to people. They point out that Wolbachia-carrying insects regularly feed on laboratory personnel with no observable health effects. The bacterium has never been detected living inside any human or vertebrate host, and while it can technically infect human cells in artificial laboratory conditions, those conditions bear no resemblance to real-world biology.
Not everyone was fully convinced. Daniel Strickman, who served as national program leader for veterinary and medical entomology at the US Department of Agriculture, expressed reservations about releasing a self-propagating biological agent that behaves differently from anything found in natural ecosystems. He specifically flagged the theoretical risk that mosquitoes rendered resistant to Dengue might become more vulnerable to other dangerous pathogens like Japanese encephalitis.
Lead researcher Scott O’Neill countered that this scenario was highly improbable, citing evidence that Wolbachia-infected mosquitoes actually showed reduced susceptibility to a broad spectrum of disease-causing organisms, not just Dengue.
Regardless of the debate around Wolbachia, the consensus was clear on one point: this bacterium-based method made genetically engineered mosquito programs largely unnecessary. The Wolbachia approach proved more effective, more economical, and significantly less risky than transgenic alternatives. Unfortunately, by the time this became evident, millions of genetically modified mosquitoes had already been released into the environment.
Oxitec’s Secret Release of Genetically Modified Mosquitoes
Oxitec engineered male Aedes aegypti mosquitoes carrying an artificial lethal gene. These modified males survive long enough to mate with wild females, but their offspring die before reaching maturity. The genetic modification is dependent on tetracycline — a widely used antibiotic — which serves as a chemical “off switch.” In laboratory settings where tetracycline is provided, the mosquitoes breed normally across multiple generations. When males are released into the wild without access to the antibiotic, their offspring inherit the lethal gene and perish.
Oxitec argued this was safe because only males were released, and male mosquitoes do not bite humans or transmit diseases. However, the manner of their field testing raised serious ethical alarms.
Millions of these genetically modified insects were released into open environments across multiple countries, with minimal regulatory review and virtually no public consultation. Oxitec deliberately selected nations with weak biosafety oversight. In 2009, genetically modified mosquitoes were released on Grand Cayman Island in what became the first-ever open-air release of GM insects capable of biting humans. The trial was conducted entirely in secret.
When residents eventually learned what had happened, the backlash was immediate and intense. Despite the controversy, Oxitec proceeded with additional releases in Malaysia, Brazil, Panama, India, Singapore, Thailand, and Vietnam. The company also sought USDA approval for open-air trials in the Florida Keys.
Oxitec reported that their modified males achieved roughly half the mating success of wild mosquitoes — sufficient to significantly suppress local populations. A 2010 Grand Cayman trial reportedly reduced the target mosquito population by 80 percent over three months. But these results came with unresolved questions about long-term consequences for both human health and broader ecosystems.
Four Critical Risks of Antibiotic-Dependent GM Mosquitoes
Neither government regulators nor Oxitec produced peer-reviewed evidence demonstrating long-term safety for their technology. Once released, genetically modified organisms cannot be recalled. Several specific risks were identified by independent researchers:
First, mobile genetic elements within the modified mosquitoes could theoretically enter human tissue through skin wounds or inhaled particulate matter. Such transfer could potentially cause insertion mutations or other forms of DNA damage with unpredictable consequences.
Second, geneticist Alfred Handler of the USDA’s Hawaii facility warned that mosquitoes could develop resistance to the lethal gene over successive generations. Entomologist Todd Shelly, also with the USDA in Hawaii, documented that 3.5 percent of test subjects survived to adulthood in laboratory conditions despite carrying the supposedly fatal modification.
Third, the sex-sorting process used to separate male from female mosquitoes before release was performed manually, with an acknowledged error rate of approximately 0.5 percent. Even that small fraction of accidentally released females could temporarily increase Dengue transmission rates while also potentially introducing modified genetic material into humans through bites.
Fourth, tetracycline contamination has been detected in soil and surface water samples across many environments. Since the lethal gene only activates in the absence of tetracycline, exposure to environmental antibiotic residues could allow modified mosquitoes to survive and reproduce indefinitely in the wild — precisely the opposite of their intended function.
The fundamental concern was that genetically modified female mosquitoes, if accidentally released, could inject the artificial protein designed to kill larvae directly into human bloodstreams during feeding, with entirely unknown biological effects.
Genetically Modified Moths and the Expanding Insect Engineering Industry
Oxitec’s ambitions extended well beyond mosquitoes. The company also developed genetically modified pink bollworm moths, which were released over agricultural fields in Arizona to combat the pest species that damages cotton crops. A genetically engineered diamondback moth (also known as the cabbage moth) was reportedly being prepared for release in England.
Other research groups were pursuing parallel programs. One team created Anopheles mosquitoes engineered to be immune to the malaria parasite, while another produced male Anopheles lacking functional sperm — both aimed at suppressing malaria transmission.
Recognizing the accelerating pace and escalating risks of insect genetic engineering, the World Health Organization began developing formal guidelines governing how genetically modified insects should be deployed in developing nations.
Strengthening Natural Immune Defense Against Dengue Fever
While the debate over engineered insects continues, individual health preparedness remains a practical line of defense. A robust immune system provides meaningful protection not just against Dengue but against the full spectrum of infectious diseases. Key strategies for optimizing immune function include:
- Eating a nutrient-dense diet emphasizing fresh organic vegetables, pasture-raised meats, organic eggs, and raw dairy while minimizing sugar, processed foods, and chemical additives — with particular attention to adequate omega-3 fatty acid intake
- Maintaining optimal vitamin D levels through sun exposure or supplementation
- Following a consistent exercise regimen
- Managing psychological stress effectively and prioritizing sufficient sleep
- Practicing thorough hand hygiene as a basic infection prevention measure
This article covers research and developments originally reported by multiple science and health journalism outlets. All facts, statistics, and scientific details have been independently paraphrased for this publication.