
The Nuremberg Code and Informed Consent
The Nuremberg Code emerged from the Nuremberg Trials following World War II, which prosecuted Nazi officials for war crimes including forced medical experimentation on concentration camp prisoners. The trials established foundational principles that continue to shape medical ethics and international law. The resulting code set forth ten principles governing permissible medical experiments on human subjects, with voluntary informed consent as its cornerstone.
The first principle states that “the voluntary consent of the human subject is absolutely essential,” requiring that the person involved “should have legal capacity to give consent; should be so situated as to be able to exercise free power of choice, without the intervention of any element of force, fraud, deceit, duress, overreaching, or other ulterior form of constraint or coercion.”

From Nuremberg to the Geneva Conventions
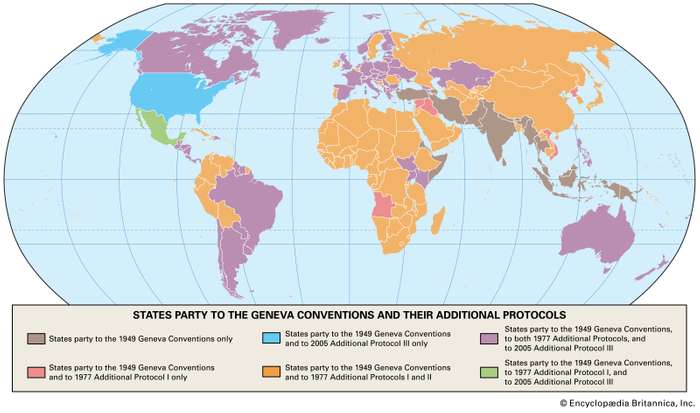
The Nuremberg Trials served as a milestone toward establishing permanent international courts and set important precedents for addressing crimes against humanity. Following these trials, the four Geneva Conventions were adopted in 1949, providing protections for wounded military personnel, prisoners of war, and civilians during armed conflicts.
In 1977, two additional protocols supplemented the Geneva Conventions. The second protocol recognized that many modern conflicts were internal rather than international, extending greater protections to combatants in civil wars and wars of self-determination.
UNESCO Universal Declaration on Bioethics and Human Rights
The 2005 UNESCO Universal Declaration on Bioethics and Human Rights built upon these earlier frameworks with provisions specifically addressing modern medical ethics:
- Article 6, Section 1: “Any preventive, diagnostic and therapeutic medical intervention is only to be carried out with the prior, free and informed consent of the person concerned, based on adequate information. The consent should, where appropriate, be express and may be withdrawn by the person concerned at any time and for any reason without disadvantage or prejudice.”
- Article 6, Section 3: “In no case should a collective community agreement or the consent of a community leader or other authority substitute for an individual’s informed consent.”

The Declaration of Helsinki
The World Medical Association’s Declaration of Helsinki established ethical principles for medical research involving human subjects. Key operational principles include:
- Article 13: Research must be subject to independent ethical review and oversight by a properly convened committee
- Article 16: Information regarding the study should be publicly available
- Article 17: Studies should be discontinued if available information indicates that original safety considerations are no longer satisfied
- Article 27: Ethical publications extend to publication of results and consideration of potential conflicts of interest
- Article 30: The interests of subjects after study completion should be part of the overall ethical assessment
The Declaration of Geneva
The Declaration of Geneva, adopted by the World Medical Association, established physician obligations including:
- The health of the patient as the first consideration
- Practicing with conscience and dignity
- Not using medical knowledge to violate human rights and civil liberties, even under threat
- Maintaining the utmost respect for human life
- Not permitting considerations of age, disease, disability, creed, ethnic origin, gender, nationality, political affiliation, race, sexual orientation, social standing, or any other factor to intervene between duty and patient
Relevant Nuremberg Principles
Several of the Nuremberg Principles adopted by the International Law Commission of the United Nations bear on questions of medical coercion and accountability:
- Principle I: “Any person who commits an act which constitutes a crime under international law is responsible therefore and liable to punishment.”
- Principle III: “The fact that a person who committed an act which constitutes a crime under international law acted as Head of State or responsible government official does not relieve him from responsibility under international law.”
- Principle IV: “The fact that a person acted pursuant to order of his Government or of a superior does not relieve him from responsibility under international law, provided a moral choice was in fact possible to him.”
- Principle VII: “Complicity in the commission of a crime against peace, a war crime, or a crime against humanity as set forth in Principle VI is a crime under international law.”
Relevant Nuremberg Code Provisions
Several provisions of the Nuremberg Code specifically address the limits of acceptable medical experimentation:
- Point 5: No experiment should be conducted where there is a prior reason to believe that death or disabling injury will occur
- Point 6: The degree of risk to be taken should never exceed that determined by the humanitarian importance of the problem to be solved
- Point 7: Proper preparations should be made and adequate facilities provided to protect the experimental subject against even remote possibilities of injury, disability, or death
- Point 10: The scientist in charge must be prepared to terminate the experiment at any stage if there is probable cause to believe continuation is likely to result in injury, disability, or death
International Legal Precedents
The United Nations Convention on the Rights of the Child, Article 19, requires state parties to “take all appropriate legislative, administrative, social and educational measures to protect the child from all forms of physical or mental violence.”
In a notable 2017 ruling, the Constitutional Court of Colombia found that mandating the human papillomavirus (HPV) vaccine was unconstitutional. The court, Colombia’s highest judicial body for constitutional interpretation, ruled that the state cannot make decisions regarding the bodily integrity of its citizens because doing so would violate human dignity. The court stressed that decisions involving medical procedures should ultimately be made by patients themselves and cautioned the Ministry of Health that informed consent must be obtained prior to administering vaccines.
U.S. Childhood Health Outcomes
A study published in the January 2018 edition of Health Affairs compared childhood mortality rates between 1961 and 2010 across the United States and 19 economically similar countries. The findings revealed that despite spending more per capita on healthcare for children than any other nation, the United States had worse child health outcomes than all peer nations studied.
Key findings included:
- U.S. childhood mortality has been higher than all peer nations since the 1980s
- From 2001 to 2010, the risk of death in the U.S. was 76 percent greater for infants and 57 percent greater for children ages 1 to 19 compared to peer countries
- American children were three times more likely to die from prematurity at birth and more than twice as likely to die from Sudden Infant Death Syndrome (SIDS)
- Over the 50-year study period, the disparity amounted to more than 600,000 excess deaths
The researchers identified premature births, SIDS, automobile accidents, and firearms-related deaths as leading contributors to the disparity and called for continued funding of programs proven to reduce childhood mortality.
The Informed Consent Principle in Practice
The legal and ethical frameworks outlined above share a common thread: the principle that individuals must have the right to make informed decisions about medical interventions affecting their own bodies. This principle was established in the aftermath of documented atrocities where populations were subjected to medical procedures without their knowledge or consent.
Whether applied to experimental treatments, vaccines, or other medical interventions, the international legal framework consistently affirms that:
- Consent must be voluntary and informed
- Individuals cannot be coerced or penalized for refusing medical interventions
- Government officials and medical professionals bear personal responsibility for violations
- Following orders does not absolve individuals of accountability
- Children deserve specific protections from physical and mental harm
These principles, forged in the aftermath of humanity’s darkest chapter, remain the foundation of medical ethics and human rights law. Their application to contemporary public health policy continues to be debated in courts, legislatures, and communities around the world.
